UPDATE July 2022: CMS is projecting PDPM reimbursement cuts in conjunction with the FY 2023 Final Rule. These cuts are in spite of the census and staffing hardships that skilled nursing facilities have endured since the beginning of the Covid pandemic. Most industry reimbursement experts feel that SNFs fail to accurately capture valuable reimbursement in the SLP Component. The elements of this article will be helpful in evaluating the speech therapy service at your building and determining if you need more expertise.
While it certainly seems like a lifetime ago since the beginning of PDPM back in 2019, we as an industry have 16-months of experience under our belts. Even though Covid has impacted most of that time frame, trends such as those in the PDPM SLP Component are beginning to emerge that are worth noting.
Nursing home speech therapists have been playing an important role in treating Covid patients as SLPs are primarily responsible for ensuring patients are on the safest, yet least restrictive diet. Adding in the respiratory distress brought on by Covid has magnified this responsibility beyond anyone’s wildest expectations.
With a sample of data on the SLP Component available, SNF operators and managers can begin analyzing these trends. Where does your SNF speech department stack up compared to your peers?
Let’s look at 4 key factors:
- Distribution of SLP Component Days – Have you looked at your building’s distribution of days? Does it make sense based on your patient population? According to Language Fundamentals Regional Manager Jennifer Maher, CCC-SLP, “the odds of a geriatric patient admitted to a SNF having some type of difficulty swallowing, history of TIA, cognitive impairment, or other comorbidity are pretty high.” Having a trained eye evaluate several months of data would be a good exercise. Here is a distribution of a large top SNF in NYS. Does your building’s distribution of SLP Component Days look similar?
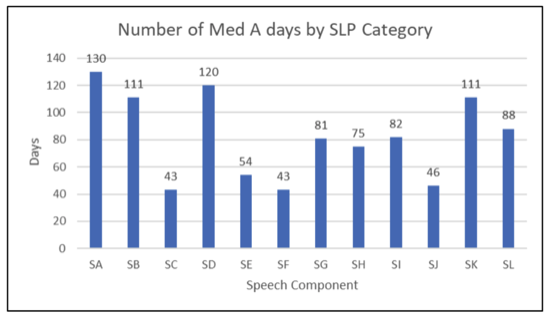
- Impact of the BIMS – Capturing impaired cognition will significantly impact the SLP Component. Is your speech department involved in the BIMS process? If not, it’s probably time to consider it. A trained medical speech-language pathologist should be a great asset to the process and will undoubtedly help you get higher and more accurate BIMS scores that will directly affect PDPM rates. Additionally, Speech-language pathologists are well suited to identify the cognitive impairment that likely exists outside of the questions on the BIMS,” according to Maher. For example, correctly capturing impaired cognition will turn an SA into an SD resulting in a $16 increase in the per diem rate.
- The “SA” Category – The SA is the lowest per diem rate (the national average $15.75. Maher says “Most SNFs will have some patients in the SA category, especially if you are treating a younger population with a shorter medical history. The key is to make certain those SAs truly belong in that category and that means understanding the SLP component inside and out.”
- Overall SLP Component Per Diem Rate – There is a great deal of dollar variation from the lowest category SA -$15.75 to the highest SL – $97.50, therefore there is a great deal at stake when ensuring the accuracy of coding. How do you know what constitutes a good SLP Component rate for your SNF & where there is an opportunity for improvement?
Would you like a complementary PDPM SLP Component analysis for your Skilled Nursing Facility? We can help. Follow the link below to get started.
Contact – Language Fundamentals (langfun.com)
SNFs that have decided to engage the organizational expertise of a specialist in medical speech therapy are far more likely to be higher performers than their peers. Are you ready to learn more?
Next month we will look at where potential audit risk lies within the SLP Component. Between the pandemic and the 1135 waiver, audits are at an all-time low. Someday when life is back to normal, external audits will soon follow. There’s no time like the present to make certain SNF Operators and Administrators are protecting themselves from future audits & potential takebacks.



